Total Shoulder Replacement
Jeff Zhao, DO | Eastern Dallas' Orthopedic Surgeon
Total Shoulder Replacement
Chronic shoulder pain can limit daily activities, disrupt sleep, and lead to a frustrating cycle of reduced mobility and increasing discomfort. When non-surgical treatments no longer provide adequate relief, a procedure known as total shoulder replacement, or total shoulder arthroplasty, may be recommended. It involves replacing the damaged surfaces of the shoulder joint with smooth, artificial components. The goal is to alleviate pain and restore functional movement.
Understanding the Anatomy of the Shoulder Joint
The shoulder is one of the most complex and mobile joints in the human body. It functions as a ball-and-socket joint. This design permits an impressive range of motion. This mobility, however, also makes the joint susceptible to wear and injury over time.
Three main bones converge to form the shoulder joint, or glenohumeral joint. The humerus is the long bone of the upper arm. Its rounded top, the humeral head, acts as the “ball.” The scapula, or shoulder blade, contains a shallow socket called the glenoid. The third bone is the clavicle, or collarbone.
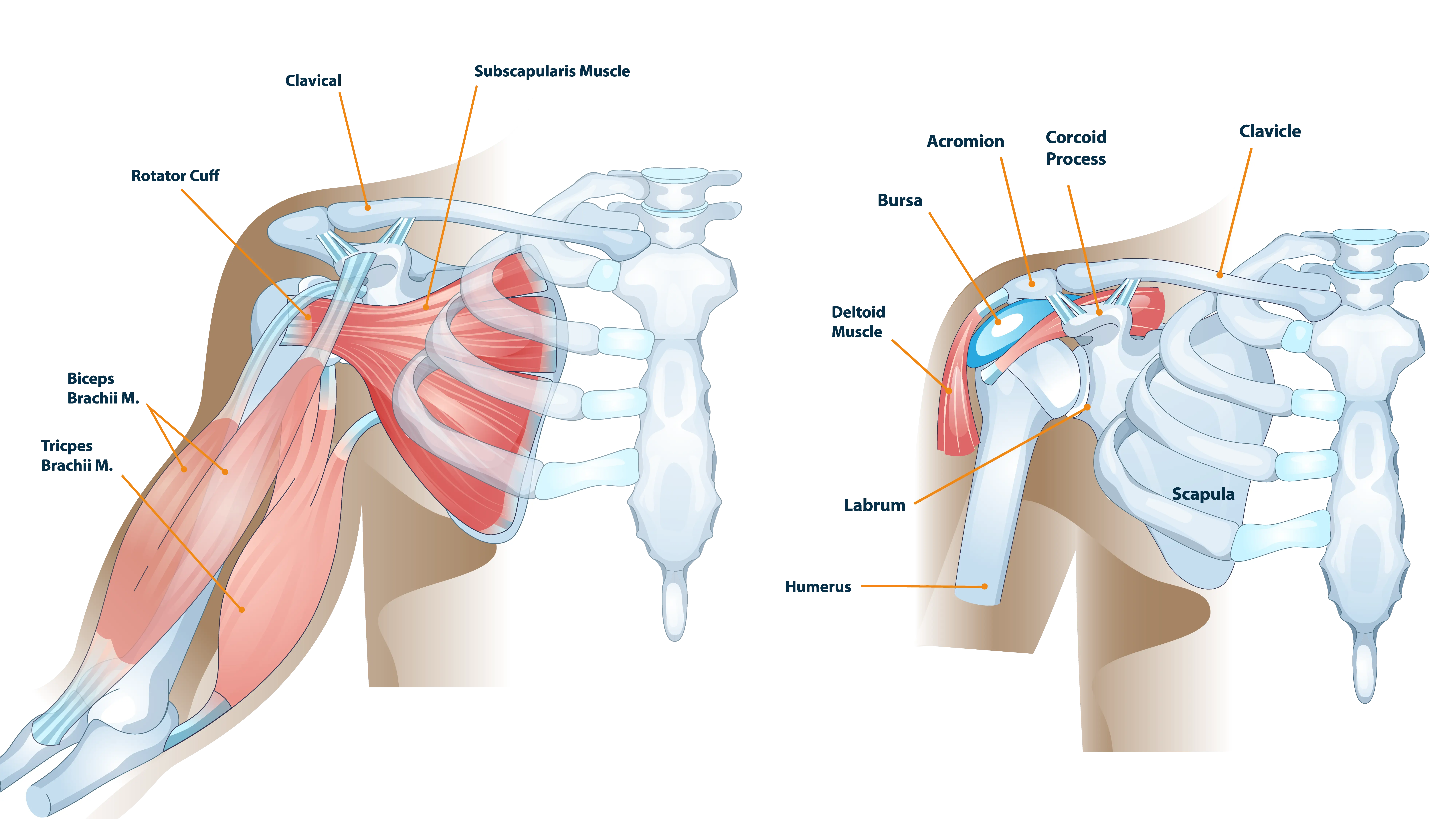
A smooth, resilient tissue called articular cartilage covers the surfaces of the humeral head and the glenoid. This cartilage allows the bones to glide against each other without friction. It ensures smooth and pain-free movement. Surrounding the joint is the rotator cuff. This is a group of four tendons and muscles that stabilize the joint and initiate movement. When any of these components become damaged, pain and stiffness can result.
When Is Total Shoulder Replacement Recommended?
A surgeon may recommend a total shoulder replacement after conservative, non-operative treatments have failed to manage a patient’s symptoms effectively. The most common reason for recommending this surgery is severe osteoarthritis. People often call this “wear-and-tear” arthritis. Over many years, the articular cartilage gradually thins and breaks down. This loss of cartilage can cause bone-on-bone friction. This friction generates significant pain and stiffness. Patients may find that their pain worsens with activity, and in some cases, it can even wake them up at night.
Several other conditions may also lead to a total shoulder replacement:
- Rheumatoid Arthritis: This is an autoimmune disease. The body’s immune system mistakenly attacks the joint lining, causing inflammation. This chronic inflammation can destroy the articular cartilage over time.
- Post-Traumatic Arthritis: A previous injury, such as a severe fracture or a dislocation, can damage the joint surfaces. This damage leads to premature wear and tear and results in arthritis.
In patients who have both advanced arthritis and a severely damaged or irreparable rotator cuff, your surgeon may recommend a different type of shoulder replacement, called a reverse total shoulder arthroplasty, instead.
The Total Shoulder Replacement Procedure
The goal of a total shoulder replacement is to resurface the damaged joint. Surgeons remove the painful, arthritic bone and cartilage. They then replace these surfaces with smooth, artificial implants to replicate the natural anatomy of the shoulder. The new “ball” attaches to the top of the humerus, and the new “socket” is attached to the glenoid bone of the scapula.

Preparing for a Successful Surgery
Preparation for a total shoulder replacement begins well before the day of the operation. A proactive approach to the pre-operative phase may contribute to a smoother surgery and recovery.
Medical Clearance and Pre-Operative Testing
Your surgeon’s office will coordinate necessary medical evaluations. These steps ensure you are healthy enough to undergo the procedure and general anesthesia. Pre-operative testing may include blood work, an electrocardiogram (EKG), and any necessary imaging tests.
Medication Management
You must discuss all prescription and over-the-counter medications with your surgeon. They will provide specific instructions on which medications to stop taking and when. Patients should also plan to pick up all post-operative pain medications and supplies before the surgery date.
Home Preparation
Preparing your home environment can simplify life during the first few weeks of recovery. You will wear a sling. You will also have limited use of the operated arm. This makes simple tasks surprisingly difficult.
- Create a Recovery Station: Set up a comfortable area where you will spend most of your time. Place the remote control, phone, books, and medications within easy reach.
- Prepare Meals: Cook and freeze several single-serving meals ahead of time. This prevents the need to cook with one arm.
- Modify Clothing: Choose loose-fitting shirts that button or zip up the front. You will find it nearly impossible to pull shirts over your head.
- Remove Hazards: Clear pathways and remove throw rugs. This minimizes the risk of a fall.
The Post-Operative Recovery Journey
Immediate Post-Operative Period
Immediately after surgery, the focus shifts to pain management and protection. Your medical team may use a combination of nerve blocks and medications to provide pain relief. The arm remains immobilized in a sling or immobilizer. This protects the healing soft tissues and the surgical repair. Patients learn safe techniques for moving and performing basic tasks with the non-operated arm.
Physical Therapy
Physical therapy is often an important part of regaining strength and mobility. While specific timelines and structures may vary, the recovery process can generally be divided into phases.
Phase 1: Protection and Passive Motion: The primary goal during this phase is to protect the surgical repair. The physical therapist focuses on passive range of motion. This means the therapist, or sometimes a machine or the non-operated arm, moves the arm without the patient engaging the shoulder muscles. The goal is to prevent stiffness without stressing the healing joint.
Phase 2: Active Motion: Once the surgeon confirms adequate soft tissue healing, the patient may progress to active range of motion. The patient now begins to move the arm using their own muscles. The therapist may also introduce light strengthening exercises. The goal is to restore independent use of the arm for daily activities.
Phase 3: Strengthening and Functional Return: This phase focuses on building strength and endurance. The patient generally begins more intensive strengthening exercises. They work toward returning to recreational activities. The therapist tailors the program to the patient’s specific lifestyle and goals.
The Long-Term Timeline
Recovery is a gradual process. It is not a sudden event. Patients should manage their expectations with patience and diligence. Often, steady improvements in function and range of motion take place over the first six months. Maximum recovery may take up to a year or even longer. Patients may continue to gain strength and refine their movement patterns well past the six-month mark.
It is important to remember that the longevity of the implant depends partly on the patient’s long-term care. Patients may be advised to avoid high-impact activities or heavy lifting. Regular follow-up appointments with the surgeon ensure that progress is regularly being checked and adjustments are made on a timely basis.
Summary
Total shoulder replacement is a well-established surgical option for patients whose shoulder pain and stiffness no longer respond to non-operative treatments. The procedure works by replacing the worn or damaged joint surfaces with smooth, artificial components. Preparing your home, managing medications, and completing all pre-operative evaluations can help set the stage for a smoother experience.
Recovery happens gradually and includes several phases of physical therapy focused on mobility, strength, and functional return. Most patients notice steady improvements within the first few months, with full recovery often continuing for up to a year or longer.
Choosing the right surgeon is an important decision you will make when evaluating treatment options. Jeff Zhao, DO, is committed to providing personalized, evidence-based care for patients considering total shoulder replacement.
Schedule a Consultation Today!


